The Painful Joint Prosthesis
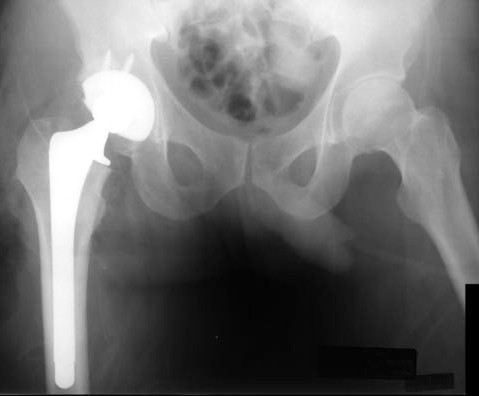
The development of prosthetic joints is a Good Thing. The alternatives include chronic, debilitating joint pain, loss of mobility and function, and even life in a wheelchair. Surgery has provided other possibilities. To paraphrase the Old Testament: “If thine joint offends thee, cast it out!” This might be the Biblical rationale for an archaic procedure called the Girdlestone procedure, in which the articular surface of an end stage, painful joint is resected. The resulting articulation can be surprisingly pain-free. Nowadays, about the only time one sees this appearance is after removal of an infected joint prosthesis or occasionally in the treatment of claw-toe deformities.
Even though prosthetic joints are a Good Thing, they are not a source of unalloyed joy to their recipients. Loosening and infection are two reasons why. There are other causes for a painful prosthetic joint, but these two items are always uppermost in the minds of orthopedists.
Why does a good prosthesis go bad? Largely because they are composed of foreign stuff that acts differently from the original bone. First of all, consider Wolfe’s Law of Bone, which is that bone is formed and retained along the lines of stress in that bone. Another way of putting it is: “Form follows function.” Look at the trabecular pattern in a calcaneus or a proximal femur — it’s easy to see where the lines of stress are here, because that’s where the trabeculae are. Another way to express this rule is: “Use it or lose it.” Bone is an amazingly dynamic tissue in this respect. Something as innocuous as spending the night in bed causes a definite but small degree of calcium loss from the bones. If one underuses a body part for a longer period, a striking amount of bone loss can be seen. A good example of this is the disuse osteoporosis seen following casting of an injured extremity. This can easily be seen on follow-up radiographs. In order to see any bone loss whatsoever on plain radiographs, one must first lose 30 – 50 % of one’s bone mass. When one considers this, the disuse osteoporosis seen after casting seems even more impressive.
What does this have to do with patients with prosthetic joints? Well, in an ideal world, a prosthetic joint component would carry stress and distribute it to the underlying bone in a manner identical to the original bone. Alas, this does not happen in real life. Prosthetic components react to stresses a lot differently than the original bone that they replaced, and tend to distribute it to the remaining bone much differently. For example, in a hip prosthesis, much of the load applied to the femoral component tends to be transmitted to the bone near its distal tip. The bone near the proximal part of the component tends to have less force transmitted through to it. What happens to the native bone that is now no longer receiving its usual loading? Bone loss occurs here. This phenomenon is called “stress shielding”. Since one can get quite a bit of stress shielding around a prosthesis, it’s no mystery why one sees progressive bone loss around prosthetic components over the years on follow-up radiographs.
The concept of stress shielding helps to explain the usual life course of a joint prosthesis. A hip prosthesis, for example, may last for 5 – 10 years before sufficient stress shielding occurs that the prosthesis loosens enough to be symptomatic. The loose prosthesis is then removed by the orthopedist, and a new one is put in. However, the native bone around the original femoral component now generally has substantially diminished bone stock. Therefore, the new one has to have a longer stem so that it will reach down far enough to seat in normal bone. This new prosthesis works for another 5 – 10 years, until stress shielding has caused enough bone resorption around this new prosthesis for it too to become symptomatically loosened. Then, a newer, even longer prosthesis is placed, and the cycle continues. Obviously, this process can’t go on forever, since you eventually run out of undisturbed bone in which to seat the prosthesis. Therefore, 20 – 30 years is about as long as one can expect to keep a series of prostheses going with a patient’s native bone stock. After that, one has to consider bone grafting. This also explains why orthopedists prefer not to put prosthetic joints into patients before they are in their 50’s or 60’s. Ideally, the last prosthesis placed should wear out about the same time that the patient does.
Life for the patient and the orthopedist would be a lot better if loosening were the only major cause of painful prostheses. Alas, life for both is much complicated by the presence of infection. For various reasons, foreign objects within the body tend to be great places to harbor infections, sort of like all of the tiny creatures living around a coral reef. One complication of infection is subsequent loosening of the prosthesis.
Unfortunately, osteomyelitis is a hard infection to treat. Despite optimal medical and surgical care, it may recur again and again over many years. This is especially true if foreign material or a devitalized fragment of bone remains in the body. This unfortunately means that an infected prosthesis must be removed. It also means that the infection must be cured before a replacement prosthesis can be inserted.
Therefore, it makes a big difference to an orthopedist whether or not a prosthetic joint is merely loosened or loosened and infected. With no infection, the prothesis will be replaced in the same operation in which the old one is removed. With infection, a new prosthesis may not be placed until several months later, once the infection has been eradicated.
The radiologist can play an important role in this decision-making. To help settle an important question like this, one needs to try to get a piece of the patient’s disease. In other words, the patient needs an aspiration-arthrogram — an aspiration of joint contents to send for cultures, and a limited arthrogram to prove intraarticular placement of the aspiration needle. In some cases, if no fluid can be aspirated, it is helpful to inject nonbacteriostatic saline into the joint to lavage the joint and then be reaspirated for culture. In my opinion, it is very important to inject at least a small amount of contrast into the joint space to prove one’s intraarticular position. In my experience, it is only too easy to inject great quantities of contrast or air into a variety of soft tissue structures (such as joint capsules, fat pads, etc.) without feeling much resistance with the injecting syringe.
Another cause of pain about a prosthetic joint is stress fracture in one of the rami of the obturator rings of the pelvis. This association is probably due to altered biomechanics following prosthesis placement. This is one of those good news/bad news findings on post prosthesis followup films. The bad news is that the patient has a stress fracture. The good news is that the patient’s pain is most likely not due to a loose prosthesis. Bursitis may also cause pain about a prosthetic joint and can clinically mimic a loosened or infected joint.
References
- Marmor L. Stress fracture of the pubic ramus simulating a loose total hip replacement. Clin Orthop Rel Res 1976;121:103-104.