Facial and Mandibular Fractures
<-Fractures Without Significant Trauma | The Painful Joint Prosthesis->
Facial Fractures
The bones of the skull and face collectively make up the most complex area of skeletal real estate in the body. Analysis of the fractured face requires a knowledge of not only normal anatomy, but also of common fracture patterns in the face.
Although they represent serious injuries, the workup and treatment of facial fractures is often properly delayed until more pressing problems have been addressed, such as the establishment of an adequate airway, hemodynamic stabilization, and the evaluation and treatment of other more serious injuries of the head, chest and skeleton. Once these problems have been managed, it is time to work up facial fractures.
At our institution, high resolution CT is currently the imaging procedure of choice for most facial fractures. The complex anatomy and fractures of the facial bones are shown extremely well by CT, and soft tissue complications can be evaluated to a far greater degree with CT. Therefore, the plain film facial series has taken a back seat to CT in the past few years, and is now used only in certain situations, such as when the facial trauma is very focal (nasal fracture), or when CT is unavailable. However I find it easier to initially teach the anatomy and fracture patterns of the face with plain films. Once these concepts have been grasped by the resident, one can then move on to the axial and coronal anatomy shown by CT.
A basic facial series consists of three or four films: a Waters view (PA view with cephalad angulation), a Caldwell view (PA view), a lateral view, and occasionally a submentovertex view. If a nasal fracture is suspected, then a lateral view of the nasal bone with special nasal technique may be done. Of these views, the most consistently helpful view in facial trauma is the Waters view. It tends to show all of the major facial structures at least as well and often better than other radiographic views of the face.
It can initially be a bit daunting to think about ruling out fractures of the complex collection of bones that make up the face. However, here are several simplifying rules that can make life a lot easier:
- Look at the orbits carefully, since 60 – 70 % of all facial fractures involve the orbit in some way. The exceptions: a local nasal bone fracture, a zygomatic arch fracture, and the LeFort I fracture. It is especially important to examine the orbital borders and apex, as well as the optic canal.
- Know the most common patterns of facial fractures and look for them.
- Bilateral symmetry can be very helpful. Normal radiopacities are usually bilateral, while abnormal ones are usually unilateral.
- Carefully trace along the lines of Dolan when examining the Waters view in a facial series.
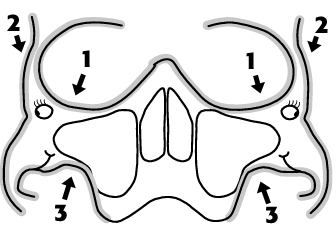
the lines of Dolan and the elephants of Rogers
What are the lines of Dolan? They are three anatomic contours best seen on the Waters view of the face, and they were first popularized by Dolan et al. As you can see, the 3 lines of Dolan lead the eye along some facially important structures. Lee Rogers pointed out that the 2nd and 3rd lines together form the profile of an elephant.
When you search for a fracture, you are really searching for one or more of the following radiographic signs.
Radiographic signs of facial fractures
- Direct Signs
- nonanatomic linear lucencies
- cortical defect or diastatic suture
- bone fragments overlapping causing a “double-density”
- asymmetry of face
- Indirect Signs
- soft tissue swelling
- periorbital or intracranial air
- fluid in a paranasal sinus
The most common mechanism producing facial fractures is auto accidents. About 70 % of auto accidents produce some type of facial injury, although most are limited to soft tissue. The face seems to be a favorite target in fights or assaults, which are the next most common mechanism. The remainder of facial fractures are produced by falls, sports, industrial accidents and gunshot wounds. Less than 10 % of all facial fractures occur in children, perhaps because of the increased resiliency of a child’s facial skeleton. The most common patterns of midfacial fractures are summarized in the table below.
| Fracture Type | Prevalence | |
| Zygomaticomaxillary complex (tripod fracture) | 40 % | |
| LeFort | I | 15 % |
| II | 10 % | |
| III | 10 % | |
| Zygomatic arch | 10 % | |
| Alveolar process of maxilla | 5 % | |
| Smash fractures | 5 % | |
| Other | 5 % | |
Probably the most common facial fracture is the tripod or zygomaticomaxillary complex fracture, so called because it involves separation of all three major attachments of the zygoma to the rest of the face.
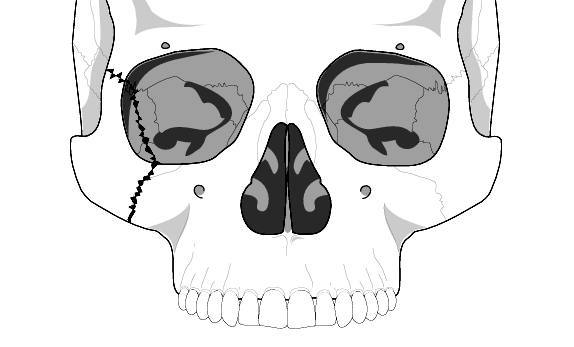
frontal view of a zygomaticomaxillary complex fracture
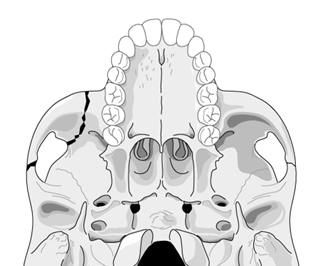
submentovertex view of a zygomaticomaxillary complex fracture
Although it may be fractured, the separation of the frontal process of the zygoma from the frontal bone usually occurs in the form of a diastasis of the zygomaticofrontal suture. This fracture is usually due to a direct blow to the body of the zygoma. This fracture will generally cause contour abnormalities of all three of the lines of Dolan. Occasionally, extraocular muscles may become entrapped in the zygomaticomaxillary component of the fracture complex. The displaced tripod fragment may physically restrict motion of the mandible. In some cases, force may propagate along the long axis of the lateral orbital wall and involve the orbital apex or optic canal, resulting in diminished vision. CT is extremely helpful in evaluating these fractures.
Fractures may be isolated to the zygomatic arch. Clinically, these injuries are usually due to a blow from the side of the face. Patients with this injury often present with flatness of the lateral cheek area and inability to open their mouth, due to impingement of the zygomatic arch fragment upon the coronoid process of the mandible or the temporalis muscle. Adequate visualization of this fracture may require a submentovertex view or CT.
Another focal fracture type is a fracture of the alveolar process of the maxilla, which involves a small piece of the maxilla, associated with several fractured teeth. The main treatment goal here is to maintain viability of the teeth. If all of the fractured teeth cannot be accounted for, a chest film should be carefully examined to look for evidence of aspirated tooth fragments.
Another common fracture is the orbital floor fracture, or “blowout” fracture. The usual mechanism is a blow to the eye, with the forces being transmitted by the soft tissues of the orbit downward to the thin floor of the orbit. The floor is usually the path of least resistance, and fractures downward into the maxillary sinus. Common clinical signs are enophthalmos and diplopia (especially on upward gaze), and one should remember that about 24 % of these fractures are associated with ocular injury as well. On a Waters view, one may see a soft tissue mass on the superior margin of the maxillary sinus, representing the herniated periorbital tissues into the sinus. One may also see a “trapdoor” fragment of bone protruding down into the sinus, often hinged on the ethmoidal side. CT will, of course, show these fractures and soft tissue mass much better.
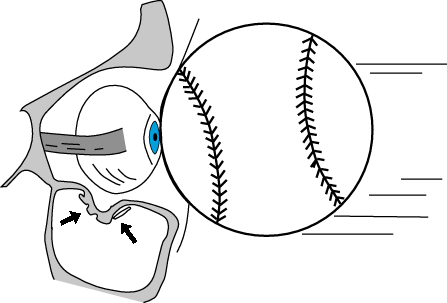
“blowout fracture” — the arrows point to the fracture fragments and periorbital tissue which have herniated into the maxillary sinus
The nose is the most frequently injured facial structure, undoubtedly because of its prominent position on the face. Likewise, the most commonly missed facial fracture of the face is a fracture of the nasal bone. Although one can occasionally see a nasal bone fracture well on a standard lateral skull film, these fractures are much better seen when the film is shot with special low kVp nasal bone technique (essentially soft tissue technique). One should always look at the inferior nasal spine (part of the maxilla) as well for subtle fractures. Common pitfalls in viewing the nasal bone are the normal sutures lining the nasal bone, as well as the linear channel for the nasociliary nerve, which may all be mistaken for a fracture. A helpful rule is that this channel runs parallel to the bridge of the nose, while most nasal bone fractures will run perpendicular to the bridge. It is well to remember that the humble nasal bone fracture may be associated with more extensive injuries, such as the orbital rim or floor and the ethmoid or frontal sinuses.
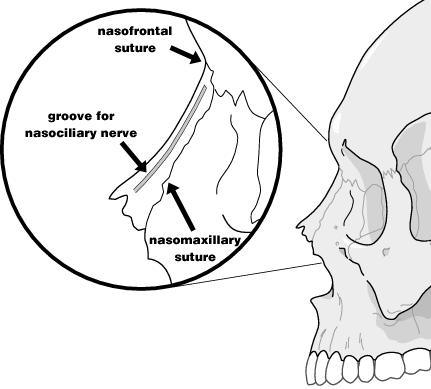
normal nasal bone anatomy
The next set of fractures in this rogue’s gallery of common facial fractures are the LeFort complexes. These are complex bilateral fractures associated with a large unstable fragment (“floating face”) and invariably involve the pterygoid plates. Legend has it that LeFort dropped skulls off of a French tavern roof and analyzed the resulting fracture patterns. This certainly sounds like the kind of study that we would all like to do, even without NIH funding. In reality, LeFort studied fracture patterns produced in cadavers. He found three main planes of “weakness” in the face, which correspond to where fractures often occur: the transmaxillary plane, the subzygomatic or pyramidal plane (this is really two planes with an apex up at the bridge of the nose), and a craniofacial plane.
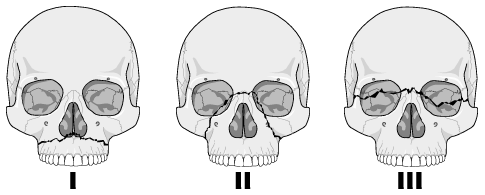
frontal views of LeFort complex fractures I – III
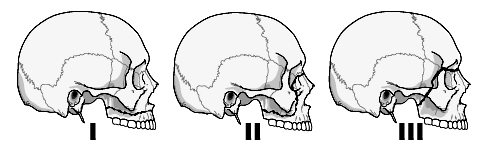
lateral views of LeFort complex fractures I – III
The LeFort I, or transmaxillary fracture runs between the maxillary floor and the orbital floor. It may involve the medial and lateral walls of the maxillary sinuses and invariably involves the pterygoid processes of the sphenoid. Clinically, the floating fragment will be the lower maxilla with the maxillary teeth.
The LeFort II occurs along yet another weak zone in the face, and is sometimes called a pyramidal fracture because of its shape. A common mechanism is a downward blow to the nasal area.
The most severe of the classic LeFort fracture complexes is the LeFort III. I suppose that this is pretty obvious, given a three-part grading system. In this case, the large unstable (floating) fragment is virtually the entire face! Thus, this fracture is also referred to as craniofacial disassociation. This is a very severe injury, and is often associated with significant injury to many of the soft tissue structures along the fracture lines. Generally, considerable force is necessary to produce this injury, and it is uncommon as an isolated injury. It may also occur in association with severe skull and brain injuries.
With the exception of the LeFort I injury, “pure” LeFort injuries are not commonly seen. More commonly seen are variants of the LeFort classification. One of the most common of these is the LeFort II – tripod fracture complex. This complex is usually due to the large forces encountered in a motor vehicle accident. LeFort was probably unable to apply this much force to the cadaver faces in his study, and it is therefore not too mysterious why he didn’t describe these more complex injuries. When describing these injuries, one should probably give a separate diagnosis to each half of the face. Even more complex patterns may be encountered, such as a mixed LeFort II/LeFort III complex or a LeFort III/LeFort II/tripod complex.
Besides the classic LeFort patterns and the mixed LeFort variants, there is another common pattern which is called, for obvious reasons, a “smash” fracture. In these injuries, severe comminution of the face is present, and underlying skull injury is likely. These patients are often in unstable condition with associated axial and appendicular skeletal injuries as well. This category includes several varieties of otherwise unclassifiable fractures, which are named for the portion of the face primarily involved. Subclassifications of smash fractures include the frontal, naso-frontal (naso-ethmoid) or central facial smash syndromes. CT is mandatory for adequately displaying all of the bony and soft tissue components of these injuries.
Wise sayings about facial fractures
- Look at the orbits carefully, since 60 – 70 % of all facial fractures involve the orbit in some way.
- Bilateral symmetry can be very helpful.
- Carefully trace along the lines of Dolan.
- Use CT liberally in working up facial fractures.
Mandibular Fractures
The mandible is another commonly fractured bone in the head, and most of these fractures are obvious on clinical exam. Clinical findings include facial distortion, malocclusion of the teeth, or abnormal mobility of portions of the mandible or teeth.
The mandible is one of those bones covered by the “ring bone rule”, which may be stated thusly: if you see a fracture or dislocation in a ring bone or ring bone equivalent, look for another fracture or dislocation. You can experiment with this tendency of ring bones to break in more than one place by going through a bag of pretzels and trying to break one of them in just one place. Then try it with a bag of bagels. You should now have a good appreciation for Lee Rogers’ corollary to the ring bone rule, which he calls the “pretzel-bagel spectrum”. To wit, the stiffer a ring bone is, the more likely it is to break in more than one place. The more flexible it is, the more likely it is to break in just one place. The mandible has some flexibility, due not only to the mobility around the temporomandibular joints (TMJ’s) but also to the tendency of the TMJ’s to absorb some forces during trauma. What this boils down to is that one sees an average of 1.5 to 1.8 mandibular fractures per customer, depending on whether the mechanism is blue collar (fist or other anonymous blunt object) or white collar (automobile crash) respectively. Like the nose, the mandible also has a prominent position on the face, making it a favorite target for either of these mechanisms. Mandibular fractures have traditionally occurred at twice the prevalence of facial fractures, but this ratio has been decreasing with the increasing prevalence of high-speed auto accidents. Only 5 % of all mandibular fractures occur in children, and most of these are also caused by auto accidents, with about 1/3 due to bicycle accidents.
Mandibular fractures can occur at any of the following sites.
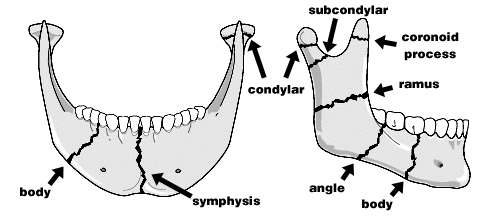
common sites of mandibular fractures
| Fracture Type | Prevalence |
| Body | 30 – 40 % |
| Angle | 25 – 31 % |
| Condyle | 15 – 17 % |
| Symphysis | 7 – 15 % |
| Ramus | 3 – 9 % |
| Alveolar | 2 – 4 % |
| Coronoid process | 1 – 2 % |
When double fractures occur, they are usually on contralateral sides of the symphysis. Common combinations include the angle plus the contralateral body or condyle. Triple fractures occasionally occur, and the most common type is fracture of both condyles plus the symphysis.
The mandible may also be dislocated without fracture, sometimes spontaneously during a large yawn. The patient usually presents with considerable pain. Spasm in the masseter and pterygoid muscles tend to force the condyles up the anterior slope of the articular eminence and prevent normal mouth closure.
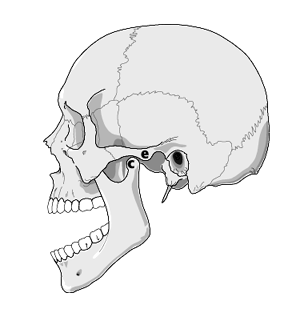
mandibular dislocation — the condyle (c) is anterior to the articular eminence (e)
Wise sayings about mandibular fractures
- Remember the ring bone rule.
- Symphyseal fractures can be diabolically hard to see, even on a well-exposed AP film
- Remember the Panorex view — this can usually only be taken by a special machine in the oral surgery department, but it provides the best single view of the mandible and will show you fractures that cannot be seen by any other method short of CT.
- Look carefully along the cortical margin of the whole mandible for discontinuities. This may be the only sign of a fracture that you will see.
- Also carefully examine the mandibular canal for discontinuities.
- A fracture line entering the root of a tooth is considered an open fracture by definition.
- Pathologic fractures can occur in the mandible. Look carefully for evidence of a periapical abscess or a mandibular tumor, especially if there doesn’t seem to be enough trauma to match the injury.
References
- Dolan KD, Jacoby CG. Facial fractures. Semin Roentgenol 1978;13:37-51.
- Dolan KD, Jacoby CG, Smoker WR. The radiology of facial fractures. Radiographics 1984;4:575-663.